Ileostomy
What is an Ileostomy?
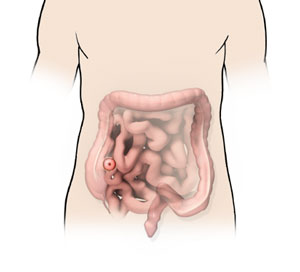
An ileostomy is a surgical procedure in which an opening is made on the abdominal wall (stoma) to connect the ileum (the lower end of your small intestine) to the abdominal wall when your colon (large bowel or large intestine) or rectum is malfunctioning or has been removed as a result of a medical condition. The stoma is connected to an externally worn pouch for collection of all the digestive waste.
Anatomy of the Small Intestine
The small intestine, also known as the small bowel, is a section that runs between the stomach and the large bowel. The large bowel is made up of the colon and the rectum. The small bowel digests food and absorbs nutrients into the blood vessels. The remaining food that cannot be digested travels from the small bowel to the large bowel. The large bowel absorbs water from the waste and reserves the waste till the next bowel movement.
Indications for Ileostomy
Your surgeon may recommend ileostomy if your colon or rectum has been affected with conditions such as:
- Colorectal cancer
- Ovarian cancer
- Ulcerative colitis
- Crohn’s disease
- A damaged or blocked colon
- Familial adenomatous polyposis
- Hirschsprung’s disease
Preparation for Ileostomy Surgery
Pre-procedure preparation for ileostomy generally involves the following steps:
- A thorough examination is performed by your doctor to check for any medical issues that need to be addressed prior to surgery.
- Depending on your medical history, social history, and age, you may need to undergo tests such as blood work and imaging to help detect any abnormalities that could threaten the safety of the procedure.
- You will be asked if you have allergies to medications, anaesthesia, or latex.
- You should inform your doctor of any medications, vitamins, or supplements that you are taking.
- You may need to refrain from supplements and medications such as blood thinners or anti-inflammatories for a week or two prior to surgery.
- You should refrain from alcohol or tobacco at least a few days prior to surgery.
- You should not consume any solids or liquids at least 8 hours prior to surgery.
- You will be placed on a special diet prior to surgery and laxatives may be used to clean out your bowel.
- You will be instructed to shower with an antibacterial soap the night prior to surgery to help lower your risk of infection after surgery.
- Arrange for someone to drive you home after surgery.
- A written consent will be obtained from you after the surgical procedure has been explained in detail.
Procedure for Ileostomy Surgery
Ileostomy surgery is performed in a hospital setting under general anaesthesia either as an open surgery where your surgeon makes a long surgical cut down your midline or as a minimally invasive laparoscopic procedure where a laparoscope – a thin, flexible, fibre-optic lighted instrument – is inserted through small surgical cuts and the necessary repair is carried out.
Based on your condition, your surgeon may perform any of the following 3 types of ileostomies.
- Standard ileostomy: This is also known as Brooke ileostomy and is the most common type. During this procedure, the end of the small bowel is pulled through the right lower section of the abdomen and attached to the outside skin. A pouch is then worn at all times to gather stool that moves through the stoma.
- Continent ileostomy: This is also known as Kock ileostomy and does not necessitate the wearing of a collection bag. During this ileostomy, your surgeon uses a section of your small bowel to create a pocket and valve system at the end of the small bowel. You can then insert a flexible tube (catheter) into the pocket to empty the collected waste as many times a day as needed.
- Ileo-anal reservoir: This type of ileostomy is also known as a pelvic pouch or J-pouch procedure. During this procedure, your surgeon makes a J-shaped pouch from the ileum and attaches it to the anus to store solid waste. The waste can then be discharged from the pouch through the anus.
Postoperative Care and Recovery
In general, postoperative care instructions and recovery after ileostomy will involve the following steps:
- You will be transferred to the recovery area where your nurse will closely observe you for any allergic/anaesthetic reactions and monitor your vital signs as you recover.
- Based on your condition and type of ileostomy performed, you may need to stay in the hospital for a few days.
- You may experience pain, inflammation, and discomfort in the operated area. Pain and anti-inflammatory medications are provided as needed.
- Antibiotics are also prescribed to address the risk of surgery-related infection.
- Walking and moving around in bed is strongly encouraged as it lowers the risk of blood clots and pneumonia. It also helps to stimulate your bowels and assist with passing gas.
- Your diet is slowly advanced after surgery. You will start with clear liquids, then pureed diet, and slowly progress to having normal solid foods, as tolerated.
- It is important to keep the surgical site clean and dry. Instructions on surgical site care, stoma care, stool collecting bag/pouch, and bathing will be provided.
- Refrain from strenuous activities and lifting anything heavier than 10 pounds for the first couple of months or until your first follow-up visit. A gradual increase of activities over a period of time is recommended.
- Eating a healthy low-fat, high-fibre diet and drinking 8 to 10 glasses of water daily is recommended to prevent constipation and for softer stools.
- Walking is a good exercise and is strongly recommended to improve your endurance.
- You will be able to resume your normal activities within a couple of weeks but may have certain activity restrictions.
- A periodic follow-up appointment will be scheduled to monitor your progress.
Risks and Complications of Ileostomy Surgery
An ileostomy is a relatively safe procedure; however, as with any surgery, some risks and complications may occur, such as:
- Internal bleeding
- Intestinal blockage
- Blood clots
- Infections
- Injury to the surrounding organs
- Inability to absorb sufficient nutrients from food