Haemorrhoids
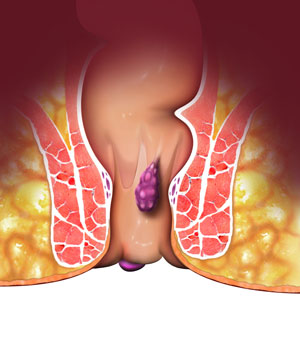
Haemorrhoids or piles or are swollen or enlarged blood vessels inside the anal canal. When veins in the lining of the anus and rectum become enlarged, they are filled with excess blood, and cause the underlying tissues to also swell, forming abnormal lumps. It occurs most commonly in individuals over 50 years of age.
Haemorrhoids are classified into two types. They include:
- Internal Haemorrhoids: These are swellings that develop inside the anus. You may not be able to see or feel them. Sometimes, they may protrude through the anus to form external haemorrhoids.
- External Haemorrhoids: These are swellings that develop outside the anus while passing stools. You may be able to see and feel them. Formations of blood clots in external haemorrhoids are called thrombosed haemorrhoids and are extremely painful.
Piles are caused due to excessive abdominal pressure from standing or sitting for long periods, being obese, pregnancy and straining during constipation. Diet plays an important role in causing and preventing piles. People who consume more processed food, and less fibre and fluids may develop piles as a result of producing hard stools and straining during bowel movements.
What are the Signs & Symptoms?
Some of the commonly occurring signs and symptoms of piles (haemorrhoids) include:
- Bleeding after a bowel movement (bright red blood)
- Prolapse of a pile through the anus
- Mucus discharge after a bowel movement
- Sore, inflamed and itchy anus
- Sensation that the bowels are not emptied completely
- Sensitive or painful lump near the anus
The symptoms usually depend on the location of the piles in and around the anus. Piles that lie inside your anal canal do not cause any discomfort, but bleeding may occur when they are irritated or while straining to pass stools. Sometimes, an internal haemorrhoid is pushed through the anus during straining, which may cause pain and irritation.
External piles may bleed and itch when they are irritated. These may also become severely inflamed, swollen and painful if a blood clot forms. The formation of blood clots in haemorrhoids is called perianal haematoma or thrombosed external haemorrhoid. External piles may form skin tags (painless soft tissue) at the edge of the anus, making it difficult to clean the anal region after a bowel movement. This increases the probability of skin infections.
Rectal bleeding may be a symptom of other conditions. Some of the symptoms such as passing black or maroon stools or blood clots may indicate bleeding at other locations in your digestive tract. In such cases, your doctor may order diagnostic tests to rule out other conditions.
What are the methods of Screening & Diagnosis?
On presenting with symptoms of piles, your doctor will conduct a thorough medical history and physical examination. Physical examination can help identify external piles that form on or around the anus. The following tests may be conducted to diagnose internal piles:
Digital rectal examination: Your doctor will insert a lubricated gloved finger into your rectum to detect abnormal growths. However, internal piles may be so small that they cannot be detected by digital rectal examination. Inform your doctor if you experience intense pain or discomfort during the procedure.
Anoscope, Proctoscope, Sigmoidoscope or Colonoscope: These scopes are flexible lighted tubes that help your doctor to view your anus, rectum, and lower colon for abnormal lumps. Your doctor may recommend colonoscopy if you are at a high risk of developing colorectal cancer or are suspected to have some other disease of the digestive system.
Some other tests include:
Biopsy: If required, a sample of tissue can be removed and sent for analysis.
Blood tests: If you experience heavy bleeding, your doctor may order blood tests to evaluate red blood cell count or haemoglobin levels.
What are the Treatment Options?
Piles usually do not require treatment as they often disappear after a few days. However, discomfort and itching may be treated with various options.
Dietary and lifestyle modifications
If the main cause for the formation of piles is constipation, the first line of treatment usually involves softening and regularising stools. The symptoms of piles can be relieved with dietary changes and lifestyle modifications. A high fibre diet, including fruits, vegetables, whole grain cereals and breads can help to soften stools and avoid straining. Your doctor will also advise you to increase your water consumption and exercise regularly to avoid constipation. Soaking yourself in warm water for 10 minutes several times a day may also provide relief.
Medications
Your doctor may suggest short-term remedies such as over-the-counter creams, ointments, or suppositories to relieve pain, swelling, inflammation and itching. Avoid using them for a longer time as they may damage the skin around your anus. Your doctor may prescribe pain killers to treat painful piles, and laxatives to soften stools and empty your bowels.
Minimal invasive procedures
Rubber band ligation: This procedure involves placing tight elastic rubber bands at the base of an internal pile. The bands cut off blood supply. This will shrink the haemorrhoid. You may experience slight bleeding after the procedure, however if you have severe bleeding you should inform your doctor immediately.
Injection (sclerotherapy): Your doctor will inject a chemical solution into the haemorrhoid. This relieves pain and hardens the haemorrhoidal tissue to form a scar. This shrinks haemorrhoids in 4 to 6 weeks. This is mainly performed in patients who are on blood thinners.
Surgical procedures
Your doctor may suggest surgery if the piles are large and are not successfully treated with other procedures.
Haemorrhoidal artery ligation: Your doctor will identify the vessel or the tube supplying blood to the piles with the help of an ultrasound probe. Blood supply to the identified vessel will be blocked with the help of absorbable sutures, which will help shrink the piles.
Haemorrhoid removal (haemorrhoidectomy): Your doctor will open the anus and surgically remove piles. This is the most effective treatment option for recurring or severe piles.